If you suspect bloat in your dog, get to the vet immediately.
Below we advise you on what you should do if your dog has bloat, based on in-depth research around canine nutrition and some experience. But it’s highly recommended that you discuss all concerns with your vet. Should you require specialised dietary advice, you can book me for a consultation.
What is bloat in dogs?
Gastric dilation (bloat) is a filling of the stomach with gas or liquid. Happens to us all and it’s usually relieved by emitting gas (in the form of a burp or fart). So far, so relieving!
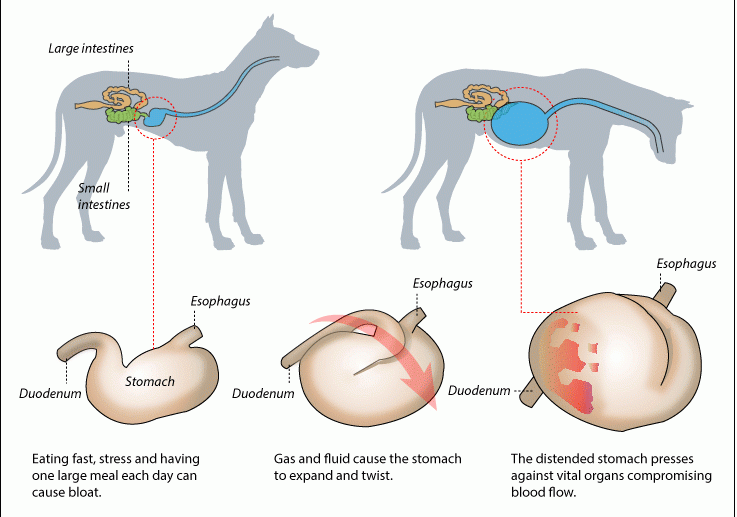
However, in some breeds and cases, when the stomach becomes severely distended without relied, pressure can be put on surrounding organs. Aside from some discomfort, should it progress, blood flow may be decreased to and from these organs. Bloat alone is rarely fatal. The problem comes when this bloated stomach decides to flip…
What is GDV in dogs?
Gastric Dilation with Volvulus (otherwise known as torsion), termed GDV, is a much more serious progression of the bloat condition in dogs. It involves the bloated stomach (and spleen, as it’s attached) suddenly twisting or flipping between 90 and 360 degrees. This seals both the entrance and exit to the stomach. As neither fluid nor gas from the digestive process can enter or leave the chamber, it builds up. If swelling continues the pain is immense and death can happen quickly. Fatality is in 15-60% of cases (Raghavan et al. 2004).
It’s important to note that while bloat often leads to GDV in dogs, as much as 85% of the time in some breeds, such as Great Danes (Neill 2015), GDV does not always arise from bloat. 58% of these pet owners who witnessed GDV in their dogs did not see any bloating whatsoever
Symptoms of bloat in dogs
The initial symptoms of canine bloat:
- the dog may be standing motionless, reluctant to sit down or he may be having trouble getting comfortable
- he may be doing a lot of stretching with his front legs head down, bum in the air
- you might hear a lot of gurgling coming from his rock hard stomach.
- he may not be in pain at this point
If canine bloat is allowed to progress:
- uncomfortable, bordering pain now and he may get extremely restless
- excessive panting
- excessive salivation
- unsuccessful attempts to vomit or defecate
The final stages of canine bloat:
- bad pain now, the stomach area may appear swollen and distended
- rapid breathing, pale-coloured gums and tongue, and collapse from shock

How to quickly check for bloat in dogs
- Make the dog stand up and you gently feel his/her abdomen.
- The abdomen should feel soft and tapered inward when the dog is relaxed.
- With canine bloat, the abdomen feels hard, and will have a hollow “thump” when gently tapped.
What to do if you suspect bloat in dogs
- Call your veterinary clinic to tell them you’re on your way with a suspected case of canine bloat so they are ready.
- The only thing you can do on the way to the vet, if he lets you, is to massage the area very gently which might manipulate the gut enough to release some gas.
- Your vet will likely pass a tube down into his stomach where a literal rush of air will escape. That is followed by washing out the stomach to remove resident debris.
- Fast the dog for 36hrs after.
This is how urgent the situation is – if you suspect you cannot get to a vet and your dog is at risk of dying, here is the advice from one of the best vets in the land, Dr. Jean Dodds:
“Whenever there is even a slight suspicion of bloat, take the dog immediately to a veterinary hospital. If is too late for that, be brave and take a clean, sharp knife and insert it quickly into the bloated side of the dog to let the trapped gas escaped from his distended stomach. This emergency procedure has saved lives – then immediately go to the closest veterinary hospital...”
I would add to this to sterilise the knife by rinsing in boiling water and allowing it to cool. If you are at the point of doing this, take solace from the fact that the dog is significantly less likely to feel the blade going in with the pain he will have in his abdomen by that time.
[Advertisement: Dr Conor Brady discusses the benefits of BioFunction 8 for gut issues in dogs]
Defining bloat in dogs – the most at-risk dog type
1. Is there an effect of breed on bloat in dogs?
Yes, most certainly. Deep chested dogs are most at risk
While it can strike any dog, it is universally accepted that bloat in dogs and particularly GDV is a major risk for larger, deep-chested dogs. A study in the United Kingdom (Evans 2010) lists the top 10 most at-risk breeds and their risk of death from canine bloat and GDV in dogs as:
- The Grand Bleu de Gascogne (21.4% prevalence of GDV; 50.0% mortality)
- Bloodhound (14.3%; 30.5% risk of death)
- Otterhound (9.0%; 7.4%)
- Irish Setter (7.2%; 5.3%)
- Bracco Italiano (5.3%; not available)
- Weimaraner (5.0%; 11.6%)
- Saint Bernard (4.6%; 15.1%0)
- Borzoi (4.5%; 9.2%)
- Italian Spinone (3.6%; 6.4%)
- Akita (3.5%; 10.7%).

The top two breeds most likely to bloat appear to be German Shepards (21% of GDV cases) and Great Danes (14% of GDV cases, Brockman et al. 1993). In a survey of 1165 Great Danes, 13% of them suffered GDV (Neill 2015).
A deep chest is most likely to feature in dog bloating (Glickman et al. 1994, Schaible et al. 1997, Schellenberg et al. 1998). In a case-control study of some 1,914 suffered bloating, a team of epidemiologists run by Glickman et al. (1994) made some interesting discoveries. Dogs with the greatest risk of developing canine bloat have chests that are deep and narrow. The depth-to-width ratio reflects the amount of room there is for stomach movement. Simply put, dogs with more room have a greater risk of developing canine bloat.
As the shape of the gut cavity is a risk factor, it should come as no surprise that Glickman et al. (2000) found that being related to a bloating dog sufferer increases their risk by 63%, suggesting a genetic basis. The effect is particularly significant for first-degree relatives (parent, sibling, or offspring, Schellenberg et al. 1998, Glickman et al. 2000b, Raghavan et al. 2004). However, a confounding factor here may be that dogs from the same pack or breeder are more likely to be handled the same way and specifically be fed the same food.
Glickman et al. (1997) and Raghavan et al. (2004) both found lean, deep-chested dogs were at greater risk. The hypothesis goes that some extra abdominal fat would reduce the amount of internal space available, working to keep the stomach somewhat in place. Supporting this, Uhrikova et al. (2015) found intact males were at greater risk of dog bloat (neutered dogs tend to put on weight) while the number of spayed females with canine bloat was significantly lower than expected (P < 0.001).
This would be the first time in my canine nutrition career where I have been made to pause over my insistence for lean dogs, but just in such at-risk breeds.
2. Is there an effect of sex on bloat in dogs?
The jury is out.
Glickman et al. (1994) further noted age was a significant factor. For large breeds, the risk of developing canine bloat apparently goes up approximately 20% each year after the age of five. For giant breeds, they found it went up 20% each year after the age of three.
This has been verified by numerous authors since (Theyse 1998, Elwood 1998, Glickman et al. 2000a, Glickman et al. 2000b). Neill (2015) did not appear to find this effect in Great Danes (when cases were expressed as a percentage of dogs in that age category, see below).

The jury is out on the effect of sex. Glickman’s analysis of 1,914 dogs (Glickman et al. 1994) found no effect of sex and this was echoed by Elwood (1998) in Red Setters and Neill (2015) in Great Danes.
On the other hand, Uhrikova et al. (2015) noted a significant difference in sex distribution with males more at risk than females (with no significant difference in sex distribution between survivors and non-survivors). Betts et al. (1974) have males at a 2:1 ratio, something that was echoed by Iowa State University Veterinary Department four years later when reviewing their cases.
It is thought male german shepherds are more at risk of canine bloat than females. I’m struggling to find a reference for that, however.
So now we have our at-risk dog – deep-chested, possibly lean, where age and being related to a sufferer increases the risk. But CRUCIALLY, this concerns a dog’s predisposition to GDV, not bloat in dogs. To put it another way, your dog’s physical shape may load the gun but it is the bloat that pulls the trigger. The question is, why are their stomachs filling with gas?

The cause of bloat in dogs
There is a lot of confusion regarding bloat and particularly torsion in dogs. Historically, a number of theories and practices have been deployed by vets and dog owners alike to avoid the dreaded situation. However, as we discuss below, many of these are without merit.
In short, a thorough review of the literature leads to this undeniable truth – the gas that fills the belly does not come from the mouth (aerophagia) but from the intestines (fermentation).
In this way, the most common cause of bloat in dogs is the consumption of foods dogs find hard to digest. Fibrous foods are a stand out here. Milk being ingested by lactose intolerants is another.
In both cases, large amounts of undigested matter make it into the large intestines, much to the delight of certain groups of bacteria that live there but usually in smaller numbers. A common by-product of these industrious microbes is gas which builds up, resulting in a fart or two in normal animals. But in these new, deep chested breeds, some can be unlucky and the gas goes the wrong way.
Here is a more thorough breakdown of what causes bloat and ultimately GDV in dogs:
The top 7 hypotheses for bloat in dogs at risk
The current hypotheses for canine bloat include:
- Meal size (volume/weight)
- Moistening the dry food
- Meal timings in relation to exercise
- Behaviour: Stress / Nervous / Anxiety
- Aerophagia (excessive air swallowing):
- Speed of eating
- Raised feeding stations
- Food Type & Water
- Gut Flora
Hypothesis 1: Does meal size affect bloat in dogs?
Meal size (by volume and weight) may be a factor.

Numerous studies of bloated dogs show that feeding a large volume of food at one time increases the risk (Glickman et al. 1997, Elwood 1998, Raghavan et al. 2004). Raghavan analysed the medical histories of 1,634 at-risk dogs. 106 suffered an attack of dog bloat. They conclude that it is the volume of food fed to large, deep-chested dogs rather than the food itself which was the problem, with the most risk coming from dogs fed once a day. This is one of the reasons owners of at-risk breeds feed smaller meals more often.
Another risk factor for canine bloat is thought to be the ligament that holds the stomach in place in the abdomen.
Hall et al. (1995) examined the hepatogastric ligaments in clinically normal dogs and GDV in dogs. They found dogs that suffered GDV had longer ligaments. From this, it was suggested that the deep-chest might permit the heavily laden stomach to stretch the ligament, allowing for increased motion and then volvulus of the stomach. The fact that the risk for gastric torsion in dogs increases with increasing age may relate to the progressive stretching of the hepatogastric ligament.
As a man that believes in questioning everything all the time and specifically here, as I have stretched and torn ligaments repeatedly in my knee from sport, I feel I need to add a thought here – it was the wrenching tackle that stretched my ligaments (which were longer after the event). My ligaments were perfectly fine going into that tackle. That the hepatogastric ligament is longer in dogs after the stomach does a flip does not surprise me. The question is, was it long in the first place? This would require measuring this ligament in a large number of healthy but at-risk dogs and waiting for dog bloating attacks to occur.
It is nearly a moot point, however. Whether you believe it is meal volume or weight, owners of at-risk breeds are covering both bases by feeding smaller meals more often (2-3 times per day) to prevent bloat in dogs.
Hypothesis 2: Does moistening the dry food increase the risk of bloat in dogs?
There is no evidence that wetting the dry meal increases bloat in dogs.

We know that dry food expands in the stomach as water is pumped in to aid digestion of the dry material. The theory goes that if meal volume is a risk factor, then pre-soaking their dry food prior to feeding should help prevent the meal from increasing in size in the stomach.
However, an unpublished analysis of 1165 Great Danes in Australia by Neill (2015) found no benefit of pre-soaking. Worse, moistening dry food prior to feeding has been found to INCREASE the risk of bloat in large-breed dogs but not in giant-breed dogs (Glickman et al. 2000).
Hypothesis 3: Meal timings in relation to exercise
Answer: There is no evidence resting after a meal helps with dog bloat

The majority of deep-chested dog owners are extremely wary about exercise post-meal. The hypothesis goes that for at least an hour after eating, the stomach is heavily-laden (it takes the average dog around an hour to reduce the meal to chyme and pass it into the intestines).
If ever canine bloat was to occur in a deep-chested dog, it would happen within an hour of dinner, right? This makes a lot of sense, hence it is readily accepted by most pet owners across forums, with some even testifying to the benefits of resting the dog BEFORE a meal, something that makes little sense to me I have to say.
Surprisingly, there is very little support for the resting hypothesis in the literature. Glickman et al. (2000) found no link between the time of exercise and bloating in dogs, whether before or after. Elwood (1998) found no effect of the duration or intensity of exercise.
To gain a little more insight here, I polled more than 110 bloated dog sufferers on my Facebook page. I asked pet owners who witnessed dog bloating in their pets, did it occur within one hour of a meal or beyond that? 80% of bloat in dogs occurred outside of the hour period, often many hours later, when the stomach is expected to be emptying into the intestines and considerably lighter as a result.
Looking at the comments from this first poll, you can see just how many owners report that the bloated dog episode appeared to happen “out of the blue”, hours after food, during rest, during sleep, during play, after a walk. It seems to happen at any time, but only 20% of the time within an hour of a meal.
Hypothesis 4: Behaviour: Stress/Nervous/Anxious
Answer: Stressed/fearful types may be at increased risk of canine bloat

You know when someone jumps out from behind a bush and gives you a good fright? Your natural reaction, if not attack them, is to clutch your chest with a sheepish laugh and say “Oh my, you gave me a fright”.
That lurch you feel in the gut is your system being flooded with the “stress” hormone cortisol. It gets you ready for fight or flight.
For both of these, your arms and legs need as much resources as possible. No time for digesting. Cortisol restricts the blood vessels around the gut, one of the most expensive organs in the body, driving all the blood to the extremities.
This is why, in periods of high stress you get a funny, IBS-like gut. If you suffer chronic stress, your poorly functioning gut results in malnutrition, losing weight over time.
This is just one of the reasons stressed children do not grow right. In this instance, it might aggravate bloat/GDV conditions.
Whenever it comes to assessments of temperament by the public or even a vet, I am overly cautious. It is plagued with issues. Still, Glickman et al. (2000) found that dogs perceived as having “happy temperaments” suffered a lower incidence of canine bloat compared to dogs that were perceived as fearful, nervous, or aggressive.
Another study found recent kenneling or something as simple as a stressful car journey predisposed dogs to a GDV episode (Elwood 1998). Other studies showed that stress in general, including agitation in response to strangers or environmental changes, were related to episodes of GDV in dogs. (Glickman et al. 1997 & 2000a). Elwood (1998) found no effect of temperament.
Hypothesis 5: Air swallowing (Aerophagia), high feed bowls and fast eaters?
Answer: Bloat in dogs is unlikely to be caused by air in from the mouth. There is no evidence high feed bowls or speed of eating is a factor.

Until recently, it was thought that canine bloat and therefore GDV in dogs was caused by too much air being swallowed by the animal (termed aerophagia). This built up in the stomach, causing bloating. Numerous studies then appeared to support this tempting hypothesis.
Glickman et al. (2000) found raised feeding stations increased the risk of canine bloat by some 200% something, the authors note, was likely due to increasing air consumption. Other authors noted that faster eaters were more likely to suffer bloat (Glickman et al. 2000). As it made such perfect sense, every effort was made to slow down the speed at which the at-risk breeds ate, but to no avail.
A fantastically useful study published by Van Kruiningen et al. (2013) examined the stomach gas of ten dogs admitted to an emergency clinic for GDV surgery. The CO2 composition of the gas was between 13 to 20%. As the CO2 concentration of the atmosphere is less than 1%, the authors could conclude that the gas is due to bacterial fermentation similar to the fermentative bloat that occurs in cattle. It was the product of fermentation from inside the gut.
In Supporting, this is the poll of more than 110 GDV sufferers on my Facebook page, 80% of attacks happened outside of the hour, just as you expect the stomach to empty into the intestines.
Re-analysis of the Glickman finding above revealed the authors had identified a correlation (giant breeds tend to use raised feed bowls under the assumption it eases the strain on the dog’s neck while feeding) and assumed it played a role in the causation. With this line of thinking, you could also worry about bigger feed bowls, bigger beds, and higher up drool marks on your clothing were all potential risk factors too.

Raised bowls are not popping up as a help OR hindrance in any other studies since. The Neill (2015) work noted that 80% of their Great Danes were fed from an elevated position. It was not found to be a common factor in their dog bloating cases. They also detected no link between speed of eating and canine bloat in Great Danes. A review of the fast-eating debate by Buckley (2016) found the evidence on speed of eating was mixed and of variable quality. She was unable to make a decision either way.
Most evidence indicates that the rate of eating has no effect on the risk of bloat in dogs. Where significant effects occur, fast eating was implicated as a risk factor. No studies found that slow eating was significantly associated with an increased risk of canine bloat. Slowing the rate at which a dog consumes a meal will not increase the risk of bloating dogs, but it may possibly reduce the risk.
Buckley 2016
Attentions, more than ever, shifted to the types of food the animal had been consuming previously.
Hypothesis 6: Food type & water
Answer: Feeding dry kibble alone increases the risk of bloat in dogs. Simply feeding “raw” is not enough to protect from canine bloat but adding in real ingredients is protective against bloat in dogs. The two chief food suspects for canine bloat are the presence of more-difficult-to-digest ingredients.

1. Does dry feeding increase canine bloat?
Numerous authors have highlighted the role of kibble in bloated dogs (Van Kruiningen et al. 1974, Kronfeld 1979, Morgan 1982). To prevent a first episode of canine bloat, their advice is to avoid feeding exclusively dry, cereal-based and specifically soy protein-based commercial dog foods.
The widespread practice of extruding dry dog food began in 1957. An epidemic of canine bloat in dogs was reported in the United States from 1965 to 1995
Raghavan et al. 2006
During the past 30 years there has been a 1,500% increase in the incidence of bloating in dogs, and this has coincided with the increased feeding of dry dog foods. There is a much lower incidence of dog bloating in susceptible breeds in Australia and New Zealand. Feeding practices in these countries have been found to be less dependent on dry foods.
Bell 2014, Tufts University
Raghavan et al. (2006) set out to examine this further. Using dry dog food label information, they checked if the risk of bloat in dogs increased with an increasing amount of soy and cereal ingredients (and a decreasing number of animal-protein ingredients) used in the food. They found no effect.
Unfortunately, the study only tested the first four ingredients, which neglects the use of some of the more fibrous and indigestible ingredients further down the ingredient list such as beet pulp and corn gluten nor was the total plant fibre content assessed. The reason for this, they cite, is their need to “balance accuracy, ease, and convenience in data collection with the need to collect data that would be meaningful and informative”. I think they missed a beat.
Plant-protein and animal protein ingredients contain non protein substances such as fibre, carbohydrates, and fat that were not accounted for in the data analysis.
Raghavan et al. 2006
2. Has raw dog food ever been linked to bloat in dogs?
I admit the above findings were more than enough to stoke my suspicions that it’s all dry foods fault (you should always start with the usual suspects). So, I again polled owners of bloating dogs on the Dogs First Facebook page asking them simply if their dogs were dry or raw fed at the time of the attack.
More than 420 responded. 77% of bloated dog patients were dry fed but 23% were raw fed. This spread is somewhat as you would expect for a ‘no effect’, considering the spread of dry to raw feeding in these large breeds is now estimated to be somewhere around 4:1 today (this is based on the fact the UK PFMA reports 10% of sales are now raw.
However, this figure does not account for the multitude of smaller businesses that are not obliged to report their sales or those feeding DIY using various non pet food manufacturer sources. We can however expect this raw figure of 24% to be inflated due to the fact I am a raw-feeding page with a raw-feeding fan base, particularly as real ingredients are seen to alleviate the harm in feeding dry food to bloating in dogs at-risk breeds.
Glickman et al. (1997) found that the addition of table foods or canned foods to the predominantly dry food diet of large and giant-breed dogs resulted in a 59% and 28% decreased risk of canine bloat, respectively. Other authors note adding fish or eggs may decrease the risk (Elwood 1998, Pipan et al. 2012).
It seems that, as ever, decreasing the amount of dry food fed to your dog, the better they will be. An epidemiological study found that Irish setters consuming a single food type were three times more likely to develop canine bloat than Irish setters fed a mixture of food types (Elwood 1998).
But still, that it happens in raw-fed dogs is interesting and implies that simply “raw-feeding”, whatever your definition of that may be, is not a suitable protector from this horrible disease. When we now know the gas is coming from internal fermentation, the attention is now very much switched to ingredients that are difficult to digest and known to increase gas in both humans and dogs.
3. Is calcium carbonate linked to canine bloat?
Raghavan above did report finding a trend of decreasing risk of dog bloating with a higher number of protein ingredients of animal origin in dry food, but this was not statistically significant (they only used 85 cases in their analysis).
On this, there are rumours in the literature that dates back to Billinghurst’s ground-breaking book “Give a Dog a Bone” in 1993, that calcium carbonate (used in dry food) is a factor.
In humans, it is used to neutralise excess acid in the stomach (think Tums for humans) as it takes a lot of acids to absorb it, reducing acid levels in the stomach. The body doesn’t just sit back and let that happen, however.
We have known for some time, (Levant et al. 1973) that small single doses of calcium carbonate (as little as 0.5g) stimulate the production of gastrin, a hormone responsible for requesting more extra gastric acid to the stomach. All this takes time, increasing the potential for a delay in gastric emptying. Normal food digestion is thus affected. It is for this reason that, compared to other calcium supplements (calcium phosphate, calcium citrate), calcium carbonate is associated with gastrointestinal side effects in humans, including constipation, flatulence, and bloating in humans.
Calcium carbonate is commonly used in dry food. Tests show many dry and canned foods are very dangerously high in calcium, with one magic “kidney” formula by Hill’s containing as much as 7.7% when independently tested (the maximum permitted is 1.6%). In fact, Thixton’s work shows many dry and canned foods made by different companies are commonly high in calcium.
Why? Because pet food relies heavily on meat and bone meal which they label “meat meal”, but is more bone than anything else (they don’t make money sending meat to rendering plants). Meat and bone meal is largely animal carcass and heads stewed up in rendering plants. As such it is approximately 30% calcium carbonate (half of your bones is calcium, give or take). This ties in with the finding by Raghavan above that “animal” ingredients are a border-line issue.
4. What about fat in food and bloat in dogs?
Interestingly, Raghavan did note that dogs fed dry foods containing fat among the first four ingredients had a 170% higher risk of developing canine bloat. This makes sense; however, their significance threshold of P=0.14 was, in my opinion, far too low for such a small sample size to make any such leap, particularly considering they stated corn was not a significant risk for bloat in dogs when its P value was a similar 0.16.
Still, the (processed) fat bit is interesting. Lena Palmer, MD, gastroenterologist, assistant Prof. in Dept. of Med, Loyola University Chicago.
Fat slows the functioning of your intestines, so if you don’t process gas very well, fatty foods could make that worse
So, perceivably, if you feed an at-risk dog the wrong diet, which increases flatulence (later), then yes, a fatty meal being held in the gut longer may increase the risk of at least bloat. Potentially.
But the fact remains, “that bit of fat off the steak” should be absolutely no problem to a normal dog. Dogs are protein and fat eating machines. They are far better with fat than we are. There is surely something else at play here.
5. What of the effect of water and canine bloat?
Some owners of at-risk dogs are wary of their pets’ water intake. Two bloated dog sufferers noted their bloating dog episode was soon after drinking a large volume of water. The role of water is absent in the literature.
There are two possible risks of water intake and bloat in dogs. First of all, drinking too much may weigh down the stomach. The issue here is that meal size by weight is not yet a risk factor for canine bloat in dogs, and I doubt a large dog would drink nearly as much water as he eats in food by weight. Further, water does not reside in the stomach too long. It passes quickly into the intestines.
However, if we run with the fermentation hypothesis, drinking too much water can certainly interfere with digestion. The body relies on stomach acids to digest your food. When you drink too much water, certainly during or soon after a meal, you dilute those acids, meaning food is less efficiently digested in your GI tract, potentially fuelling the growth of the wrong bacteria. Gas and or bloating may result. And as we know, high salt dry food makes you drink a lot of water, particularly after a run.
Hypothesis 7: The gut biome
A study by Hullar et al. (2018) of Great Danes with canine bloat found the patients had a significantly more diverse faecal microbiome than healthy control dogs. Dogs with canine food bloat showed a greater number of Actinobacteria and Firmicutes and a significantly lower abundance of Bacteroidetes.
This is interesting and somewhat as you would expect based on studies of humans which reveal the very same bacteria (Firmicutes and Actinobacteria) are among the chief culprits for increased gas production in humans (Manichanh et al. 2013). In fact, these authors wanted to test the effect of their “flatulogenic diet” on healthy human patients.
This diet was based on a greater intake of more fibrous items, including whole grains, beans, soya, as well as a variety of fibrous fruit vegetables, including good old cruciferous vegetables (Brussels’ sprouts, cauliflower, broccoli, cabbage).
This calls into question the modern use of legumes (peas, lentils etc…notorious for causing gas) in grain-free pet foods.
The Hullar work supports the hypothesis that there may be immunogenicity to bloat in dogs, one that is kicked off by a gut microbiome imbalance (or dysbiosis). The gut biome in dogs is intricately linked to how their immune system fires. Further research is urgently required here.
The most likely cause of bloat in dogs, in conclusion…
There is currently no scientific consensus on this one. Where there isn’t, you understandably get a lot of people recommending different things. My tuppence worth is that breed, shape, and age alone are not enough to explain canine bloat, or more dogs would be suffering from it.
Some environmental factors are causing large amounts of bloat gas in certain dogs. A review of the literature strongly indicates it is the fermentation gas from improperly digested food items. This is based on:
- Studies show dry food is a chief food suspect. Dry food is not only packed with chemical antimicrobials, which not only negatively affects life on the food but also disrupts the life in your dog’s intestinal tract. It is often too high in calcium carbonate and uses fillers such as wheat gluten and indigestible plant fibre fillers such as corn gluten and beet pulp that are expected to fuel bacterial growth and thus gas production. If you want to help avoid canine bloat, stop feeding dry food.
- Bloat in dogs is unlikely to be caused by aerophagia. We now know the gas is not atmospheric, it is coming from the inside
- The recent biome work confirms bacterial disruption.
- Volume of food is a factor. The more (incorrect) food going in, the more fermentation gases produced at one time.
- My poll of more than 110 sufferers revealed 80% of attacks are happening outside of an hour when the stomach is emptying into the intestines.
Best advice for preventing canine bloat
If I had an at-risk breed, I would be doing my best to maintain a healthy gut flora in my dog. This means:
- Stop feeding dry food or chemically preserved pet store treats.
- Feed your at-risk dog a raw dog food diet.
- Feed 2-3 smaller meals rather than 1 large meal in case of an upset, certainly when transitioning between new flavours.
- Conduct a well-run exclusion diet to detect any dietary issues he may be having with one or two proteins. Consider a saliva test to help you identify problem proteins for your dog (the one I link to is only $100 and tests over 250 different foods. Saliva tests are not definitive but a great pointer).
- While I am normally a fan of some plant additions in dogs, with canine bloat in mind, at-risk owners should consider the amount of plant fibre they are feeding their dog. At least par-cooked plant ingredients to break down plant fibre. I would avoid cruciferous vegetables, beans etc.
- Do not feed any fermented veg until we know more about their effect on gas production in dogs
- Avoid feeding any fruit (fermentable)
- Bins must be inaccessible at all times
- Be wary of antibiotics and always couple with probiotics
- Be very wary of NSAID’s, they are notoriously bad for guts (and they alter the gut flora). If your large breed is suffering from arthritis there is lots you can do naturally before these drugs are considered.
- Use faecal checks over chemical worming
- Take good quality canine probiotics. I don’t have a preference here really.
- Remove chlorinated water (disrupts guts). Charcoal sticks in a tub of water do the job though a decent filter will save you a lot of trouble.
I would suspect that quick changes in diet may disrupt their gut flora (bin raiding often results in a canine bloat attack). When moving your dog from dry to raw dog food, do it carefully. I would probably feed a lightly cooked mixture for a time (slightly easier to digest) before slowly moving to raw. Use digestive enzymes for the whole transition to ensure the digestive process is firing full whack.
You want regular bowel movements, this should be achieved with the right diet. Some at-risk owners recommend adding fibre to aid this process. I would not do this, it may feed the wrong bacteria. The best carnivore fibre is hair and hide so maybe pick up your at-risk breeds some hairy rabbit ears.
In line with the best practices of Zoo Pharmacognosy, try growing some peppermint (very impressive antispasmodic of the gut, IBS sufferers use it a lot) in a little pot which he can access should he need it. And they do.

I would have to hand out a few items that might work to reduce gas, should I sense my dog is suffering from gas, such as Simethicone (I am told), but to be clear, I would not include these daily in my dog’s diet. All these products have side effects too, including messing with your biome. They are a plaster on gangrene.
I have heard some owners of at-risk breeds recommend small amounts of charcoal daily. I don’t know but a word of caution – while charcoal can bind gases from the intestinal tract (yay), used excessively it may also slow the passage of digesta and constipate you over time.
What about Gastroplexy? This is the stitching of the stomach to the abdomen wall to prevent movement. All I can say is that studies show it is effective as a long term solution for gastric torsion in dogs. I just don’t know of the long-term side effects.
That’s all I have. This is a real shocker of a disease and far too common in the canine population. We must get on top of this one. Very best of luck to anyone living with the threat but take solace that there are surely things you can do to reduce the likelihood of this occurring. A few more years of data from the top raw feeding vets will reveal that the above diet advice will surely reduce fermentation gases and thus canine bloat and thus risk of GDV in your beautiful but at-risk, deep-chested dogs.
I have spent a lot of time building up my knowledge. From a doctorate in animal behaviour and nutrition to years in guide dogs and the last seven years inside and out of the pet food industry, I have always provided all my information free to the public, articles that I spend a lot of time putting together. While it’s clearly a passion of mine the fact remains, I can’t do this and a steady job at the same time. Without a salary or fancy sponsorship, I am left trying to monetise my site as much as I can without pushing on you horrible adverts for car loans and crap pet products. One way I do this is by tracking some of the links to products I recommend. Another is by popping a few ads for my products in some of my bigger articles. Finally, I’m now putting a donation button at the bottom of my more helpful articles. So, if this helped you in any way, fixing your dog where repeated vet visits have failed, and you feel you’d like to give me the price of a cup of coffee, please feel free to do exactly that. If you’re strapped and can’t afford it, I can totally sympathise, you’re free to read on, no questions asked. We’re glad to have you on board spreading the word regardless.
References Used for Bloat in Dogs
Bell, J.S. (2014). Inherited and Predisposing Factors in the Development of Gastric Dilatation Volvulus in Dogs. Topics in Company An Med. An excellent review.
Betts, C. W., et. al. (1974). A Retrospective Study of Gastric Dilatation-Torsion in the Dog. Journal of Small Animal Practice. 15: 727-734
Kronfeld D. (1979). Common questions about the nutrition of dogs and cats. Compend Contin Educ Prac Vet;1:33-42.
Levine M, Moore GE. (2009). A time series model of the occurrence of gastric dilatation-volvulus in a population of dogs. BMC Vet Res 5:12 Moore GE, Levine M, Anderson JD, Trapp RJ. Meteorological influence on the occurrence of gastric dilatation-volvulus in military working dogs in Texas. Int J Biometeorol 52:219–222, 2008
Morgan RV. (1982). Acute gastric dilatation-volvulus syndrome. Compend Contin Educ Prac Vet;4:677-682
Neill (2015). Australian Great Dane Health and Lifestyle Survey. Published online.









